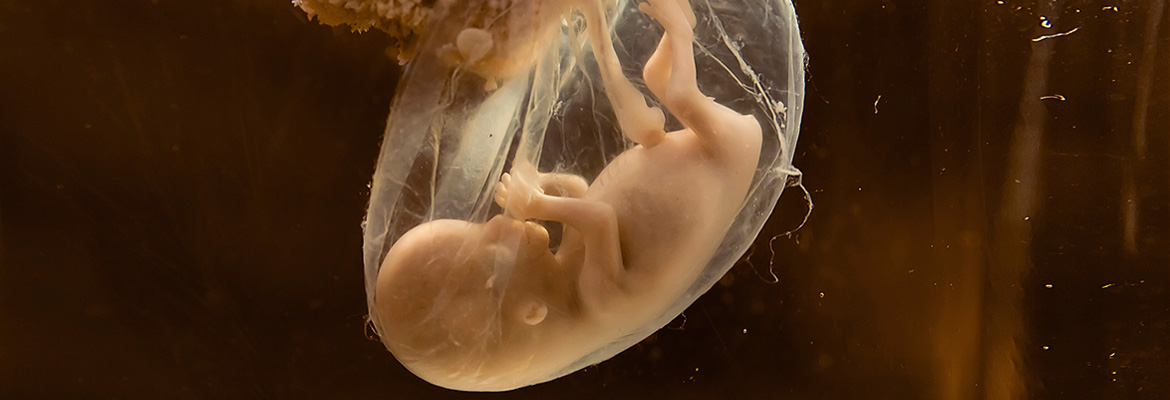
In 2012 more than 10 percent of births in the United States were preterm, and nearly 1 percent of births were critically preterm (younger than 26 weeks). These numbers point to a sobering truth: every year, hundreds of thousands of babies are born before they’re ready, requiring urgent medical care immediately after (and likely during) birth.
Coming into the world too early can lead to myriad health issues. Preterm babies, particularly those born before 28 weeks, face a host of challenges, including the fight just to survive. And preterm babies don’t just face health challenges in the hours and days following their births — many are confronted with obstacles throughout their lives. Those infants who do survive may experience temperature fluctuations, respiratory issues, gastrointestinal and cardiovascular problems, and neurological problems like abnormal blood vessel development, or damage and scarring of blood vessels in the retina.
But investigators at The Children’s Hospital of Philadelphia are on the cusp of an innovative approach to caring for these most delicate infants, one that could radically transform the way they are treated and significantly improve their outcomes.
Alan W. Flake, MD, an attending surgeon and director of the Hospital’s Center for Fetal Diagnosis and Treatment, has been leading a groundbreaking project on the development of an extracorporeal support of the premature infant (ESPI) system. Far more than a standard incubator or isolette, the device Dr. Flake’s team has been developing is exactly what it sounds like: an external uterus designed to help preterm infants bridge the gap between their mother’s womb and the world.
A key member of Dr. Flake’s team is one of the project’s biggest champions, Emily Partridge, MD, PhD, a research fellow in the Center.
Dr. Partridge’s experience during her OB/GYN rotation inspired her to work to improve outcomes for preterm infants. She witnessed the birth of a 21-week-old infant who was born early because of the mother’s health issues, despite the fact that the baby was otherwise healthy. Because the baby was so young, “There was really nothing that could be done,” Dr. Partridge said. “It’s just the most frustrating thing . . . it’s quite awful.”
And those preterm infants who are old enough to be born at 24 weeks have numerous problems. “Even the babies who do survive sometimes have quite catastrophic injuries because of the relative immaturity of their organs and the fact that, at a very simplistic level, they’re just not ready to be out here yet,” Dr. Partridge added.
The concept for a device that could improve outcomes for preterm babies is not new, as the idea for an external uterus has been around since the 1960s. Indeed, the work of Children’s Hospital’s own William J. Rashkind, MD, indirectly contributed to the ESPI project. The former chief of the Division of Cardiology, Dr. Rashkind was a balloon catheter and artificial lung pioneer who led a study in 1965 that showed the viability of a pumpless oxygenator in children with respiratory failure. His study was one of several integral to the development of extracorporeal membrane oxygenation (ECMO), which is designed to give respiratory and cardiac support to critically ill patients. However, ECMO is generally contraindicated in infants with gestational ages less than 34 weeks and weighing fewer than 2,000 grams.
Building on elements of other designs and previous work, Drs. Flake and Partridge — as well as team members Holly L. Hendrik, MD; Marcus Davey, PhD; and Kevin Dysart, MD — have been working on a device that is designed to mimic the intrauterine environment by allowing neonates to breathe fluid (as opposed to a traditional incubator’s gas) while promoting growth and organ development.
“We’ve tried to mirror what would be happening in utero,” Dr. Partridge noted.
The ESPI device started as a glass incubator tank combined with monitoring devices, but has since evolved into a plastic bag with an incorporated oxygenator and a continuous amniotic fluid exchange system. The fetus — or in this case, the preterm lambs with which the researchers have been working — rest in the device. Lambs have long been the model animal for fetal surgery research, Dr. Partridge noted, because they are roughly the same size as human fetuses and exhibit similar fetal movements.
Within their bags, the lambs are supported by a water pillow in a temperature-controlled environment, with cannulas running into and out of the bag to the pumpless oxygenator, amniotic fluid exchange system, waste removal system, and other ports for a variety of monitors. Vital signs, blood flow, fetal blood gases, and other parameters are continuously monitored in the ESPI system. And by using a pumpless system, the fetus’ heart acts as the pump, as it does in the mother’s uterus.
Despite the challenges of supporting a fetus in a sterile environment outside the womb and the huge engineering and circulatory challenges posed by ESPI, the project has been enormously informative — and successful. In addition to making great strides toward designing “a perfectly closed system,” the research team has learned a number of things about how the placenta functions and are turning their attention to questions about how fetuses and their mothers interact, Dr. Partridge noted.
Going forward, Dr. Flake and his team will study the viability of their system in increasingly preterm lambs, and will work to improve the system’s design. They also plan to further study fetal metabolism and growth, and they hope to expand their work to include models of diseases like congenital diaphragmatic hernia, a condition in which a hole in the diaphragm fails to close during development.
“I truly believe that this is the future of how preterm infants will be cared for, that one day you’ll see rows of bags in the NICU,” Dr. Partridge said. Added Dr. Flake, “This is an enormously promising study. Our system is designed, as much as possible, to avoid the deleterious effects of preterm birth.”
Perhaps one of the most promising approaches to cancer treatment lies in immunotherapy, which involves harnessing the body’s immune system to attack tumors.
By carefully adjusting the function of these crucial immune cells, Children’s Hospital investigators may have developed a completely new type of cancer immunotherapy. To accomplish this, they had to thread a needle in immune function, shrinking tumors without triggering unwanted autoimmune responses.
The new research, performed in animals, is not yet ready for clinical use in humans. However, the approach, which makes use of a key protein to control immune function, lends itself to further study using candidate drugs that employ the same mechanisms.
“There’s a basic paradox in immunology: Why doesn’t the immune system prevent cancer in the first place?” said the study’s leader Wayne W. Hancock, MBBS, PhD, chief of the Division of Transplant Immunology.
The answer is complicated, but much of it involves a delicate balancing act among elements of the immune system. While immunity protects us against disease, an overly aggressive immune response may trigger dangerous, even life-threatening, autoimmune reactions in which the body attacks itself.
In the study, published in Nature Medicine, Dr. Hancock and his colleagues focused on a subtype of immune cells called Foxp3+ T regulatory cells, or Tregs. Tregs were already known to limit autoimmunity, but often at the cost of curtailing immune responses against tumors.
“We needed to find a way to reduce Treg function in a way that permits antitumor activity without allowing autoimmune reactions,” Dr. Hancock said.
The investigators showed that inhibiting the enzyme p300 can affect the functions of another protein, Foxp3, which plays a key role in controlling the biology of Tregs. By deleting the gene that expresses p300, the researchers safely reduced Treg function and limited tumor growth in mice. Notably, they also achieved the same effects on p300 and Tregs by using a drug that inhibits p300 in normal mice.
“The study demonstrated proof of principle that using a drug to regulate the function of a special, immunosuppressive subset of Treg cells safely controls tumor growth,” Dr. Hancock said. “It really moves the field along toward a potentially major, new cancer immunotherapy.”
Dr. Hancock plans to pursue further investigations into targeting p300 in immunotherapy. The preclinical findings offer encouraging potential for being translated into the clinic, Dr. Hancock said, who added that pharmaceutical companies have expressed interest in researching this approach as a possible cancer therapy.
The antitumor study, down-regulating Treg function, is the flip side of another part of Dr. Hancock’s Treg research. In a 2007 animal study, also in Nature Medicine, he increased Treg function with the goal of suppressing the immune response to allow the body to better tolerate organ transplants. In the current study, decreasing Treg activity permitted the immune system to attack an unwelcome visitor — a tumor. In both cases, he relied on epigenetic processes — using groups of chemicals called acetyl groups to modify key proteins — but in opposite directions.
“This is the yin and yang of immune function,” Dr. Hancock noted.

A compelling approach to targeted delivery of drugs in pediatric oncology aims chemotherapeutic agents more selectively in order to give less total drug and get much more effect. Researchers at The Children’s Hospital of Philadelphia are formulating ways to pack this punch into biodegradable nanoparticles — 100 times smaller than red blood cells — to help treat patients with neuroblastoma.
A tumor of the sympathetic nervous system, neuroblastoma has lagged behind cure rates for other solid tumors of childhood. It accounts for 8 to 10 percent of all childhood cancers and 15 percent of deaths from cancer in children, as the majority of patients have advanced metastatic disease. Few new treatment agents are in the pipeline, so researchers are concentrating on how to improve the performance of more conventional anticancer chemotherapeutics in new ways.
Garrett M. Brodeur, MD, acting director of CHOP’s Center for Childhood Cancer Research, and a member of the Division of Oncology at CHOP, together with a team of cardiology researchers, Michael Chorny, PhD; Ivan Alferiev, PhD; and Robert Levy, MD; have studies under way that use nanoparticles as delivery vehicles for SN38-TS, a precursor of SN38. SN-38 is a cytotoxic agent which cannot be administered as is, and is currently delivered in the form of another precursor (also called a “prodrug”) irinotecan, used as a treatment for recurrent or resistant neuroblastomas.
A prodrug is a compound that becomes an active drug in the body. Unlike irinotecan, the prodrug design of SN38-TS was adjusted for incorporation into biodegradable nanoparticles finely tuned by the researchers as tumor-targeted delivery vehicles.
“We are taking a uniquely integrated prodrug/nanocarrier-based approach where all formulation components work together to effectively deliver the therapy,” Dr. Chorny said. “SN38-TS is designed to travel with the nanoparticle, get released at a slow rate directly in the tumor, and become converted into the pharmacologically active drug rapidly. This way, we can take advantage of the tumor-targeted delivery to the highest possible extent.”
Using mouse models, the research team has demonstrated that lower total doses of the nanoparticle-delivered drug, SN38-TS, can kill tumors more effectively and with less toxicity than conventional delivery of irinotecan.
“This is huge because irinotecan has a narrow therapeutic window, which is the difference between the lowest dose you can give to kill the tumor and the highest dose before it exerts serious short- and long-term adverse effects,” Dr. Brodeur said. “Now we can take that window and open it to the ceiling because we can get 10 to 100 times more drug into the tumor by using these nanoparticles as drug delivery vehicles while exposing the patient’s systemic circulation to much less of the drug.”
This nanocarrier formulation protects the active agent, SN38, from inactivation, and its controlled release once inside the tumor tissue enables its accumulation and protracted presence at therapeutically effective levels. The drug is exposed to healthy tissue less because it is entrapped in the nanoparticles while it is circulating. Also, as opposed to irinotecan, it does not need to be metabolized by the liver to be activated.
The administration of SN38-TS in its nanoencapsulated form allows it to take advantage of a principle called the EPR effect, which stands for “enhanced permeability and retention.” Dr. Brodeur explained how it works:
Normal blood vessels have tight junctions between the cells, so very little can get between the cells and into normal tissues. On the other hand, tumor blood vessels are leaky. Nanoparticles in a specific ultrasmall-size range (less than 100 nanometers) will pass by the normal cells and tissues and accumulate in the tumor. Tumors also do not have an efficient circulatory system, so the nanoparticles are retained in the tumor longer.
“That plays to our advantage in terms of the nanoparticles because we can get drug in, have it slowly break down in the tumor, and then we can expose the tumor to more drug,” Dr. Brodeur said.
Drs. Chorny, Alferiev, and Levy are experts at designing the nanoparticles so that they are the ideal size and composition. If they are too big, macrophages from the patient’s liver and spleen will identify them as foreign, like a virus, and eliminate them, so exposure to the tumor is limited. If they are too small, they could enter normal tissues, just like the free drug. As in the fairytale Goldilocks, the nanoparticles cannot be too big or too small; they must be just right.
The researchers use polymeric nanoparticles, which are chains of polymerized lactic acid. Polyethylene glycol is added to make them stealthy so that the patient’s immune system does not recognize them easily. These components also are completely biocompatible and bioeliminable.
“They are simple molecules that are fairly easy and inexpensive to make,” Dr. Brodeur said. “They are very effective at doing their job, and then they just break down.”
Dr. Brodeur anticipates that the SN38-TS nanoparticle formulation may be ready to be tested in clinical trials as early as the end of 2015.
“We think the potential application is great, not just for neuroblastoma patients, but to any patient who you might treat with irinotecan, so that includes a number of other solid tumors in children and adults,” Dr. Brodeur said.
In the future, nanoparticle formulations could be created for other drugs, and this has important implications for tumors that currently are considered to be natively resistant. The research team also will explore the nanoparticle delivery of co-drugs that may be synergistic when given together, and they will try pairing nanomedicines with conventional drugs to see if they have a combined effect.

Prophylactic antibiotics are prescribed to prevent – rather than treat – the spread of bacteria that can lead to serious and, at times, life-threatening, infections.
Many patients with vesicoureteral reflux (VUR) who suffer from a urinary tract infection often receive the antibiotics daily, and they must take them for years to prevent infection. About 5 percent of children will have a UTI by age 6, and approximately one-third of these patients have VUR. When a child with VUR urinates, some urine backs up in the ureters toward the kidneys and therefore the bladder does not empty completely. This increases the chance of a UTI and, if the urine reaches the kidneys, it is often accompanied by a fever and is called pyelonephritis.
“The problem with pyelonephritis is that it sometimes results in kidney scarring, and there is a concern that this could lead to high blood pressure and renal failure when you get older,” said Ron Keren, MD, MPH, who was a co-investigator on a multisite clinical trial on the use of prophylactic antibiotics to prevent UTIs in children with VUR.
Clinicians currently use either a long-term course of daily antibiotics or antireflux surgery to treat children with VUR. However, an international clinical study conducted in the 1980s showed no difference in the rates of recurrent UTIs or renal scarring between the two approaches. More recent trials that looked at antibiotics’ effectiveness had conflicting results and methodological weaknesses, so researchers launched the Randomized Intervention for Children with Vesicoureteral Reflux (RIVUR) trial to obtain more evidence to guide clinical practice.
Dr. Keren and his fellow investigators on the RIVUR trial studied 607 children from 19 clinical sites across the U.S. and followed them for two years. They poured through data to determine if children who received daily doses of the antibiotic trimethoprim-sulfamethoxazole had fewer recurrences of UTIs than those who received the placebo. They also looked to see if there were any differences in the occurrence of renal scarring.
The results of the study were “pretty dramatic,” Dr. Keren said.
The research team found that those who received prophylactic antibiotics had their chance of developing a UTI cut in half. The percentage of children getting UTIs increased over time in the placebo group but not in the treatment group, Dr. Keren pointed out, which demonstrated the sustained effectiveness of the antibiotic.
The investigators, who published their study in the New England Journal of Medicine, also found little difference between the treatment and placebo groups when it came to renal scarring.
Dr. Keren said he was surprised that the prophylactic antibiotics worked as well as they did, although he cautioned that the team’s finding about renal scarring will likely add fuel to the ongoing debate about the use of prophylactic antibiotics.
“Some physicians will say it is not worth using daily antibiotics in children with VUR if they don’t prevent kidney damage,” he said. “Others will say it is important to continue to treat these children with antibiotics because a UTI recurrence could land them in the emergency room or hospital.”
The findings in the RIVUR study will likely affect the use of urinary tract imaging — called voiding cystourethrogram (VCUG) — to screen patients for VUR. While the imaging can be a helpful diagnostic tool, it involves radiation exposure and is invasive, uncomfortable, and often traumatic for children. The current guidelines recommend that physicians take a watchful waiting approach before suggesting the procedure. Part of the rationale for this approach was the lack of strong evidence for the effectiveness of prophylaxis in children with VUR.
Now that we know that prophylaxis works, this may change the calculus for some providers about the risks and benefits of getting a VCUG on every child who has a first UTI, though the American Academy of Pediatrics still recommends waiting for a second UTI, as the majority of children will never have another one, Dr. Keren said.
With so many ongoing discussions about the best ways to approach UTIs, the issue is ripe for further research. Dr. Keren is involved with another NIH-supported study that follows a design similar to RIVUR, known as the Careful Urinary Tract Infection Evaluation (CUTIE) trial, but it is focusing on the rate of recurrent UTIs and kidney scarring in children who do not have VUR.
Children’s Hospital investigators continue to be on the forefront of pediatric medicine, as evidenced by two new awards from the Patient-Centered Outcomes Research Institute (PCORI). The awards, which aim to support the development of a data network and a landmark study of antibiotics, draw on the Hospital’s large repository of health data and on its sprawling regional network of healthcare providers.
PCORI was established by the Affordable Care Act to fund and carry out comparative effectiveness research, which compares healthcare approaches currently in practice to determine which approaches are the most effective and beneficial. Since PCORI began funding research projects in 2012, the organization has been awarded a staggering $464 million to support 279 projects.
In September 2013, Jeffrey S. Gerber, MD, PhD, received an approximately $1.8 million contract from PCORI to compare the effectiveness of broad- and narrow-spectrum antibiotics in treating acute respiratory infections. An infectious diseases specialist and a faculty member in the Center for Pediatric Clinical Effectiveness, Dr. Gerber investigates the epidemiology and outcomes of antibiotic use in children.
Dr. Gerber’s three-year investigation focuses on the use of antibiotics to treat acute respiratory tract infections (ARTI), such as ear and sinus infections. Despite the fact that guidelines frequently recommend clinicians use narrow-spectrum antibiotics to treat ARTI, many doctors often prescribe broad-spectrum antibiotics.
“Using parent- and patient-centered outcomes, this study is designed to identify which antibiotic choices best optimize clinical outcomes while minimizing side effects,” Dr. Gerber said. In addition to assessing traditional medical outcomes, the investigators are seeking to gauge “outcomes that aren’t typically on a medical chart” — like diarrhea or absence from school, which may not require a visit to the hospital but can be disruptive for patients and families, Dr. Gerber said.
Between 2006 and 2008, there were approximately 65.6 million doctor visits for respiratory conditions, according to a 2011 Pediatrics study. During those 65.6 million visits, there were 31.7 million antibiotic prescriptions made.
While prescribing antibiotics can be challenging for general practitioners, the guidelines are relatively straightforward for antibiotic prescribing for the most common conditions that affect kids: ear infections, strep throat, sinus infections, and pneumonia, Dr. Gerber said.
The possible implications of the project are extensive, as antibiotic prescribing and ARTI are so widespread. “Given that these four conditions account for 80 percent of antibiotic prescribing, and given that outpatient antibiotic prescribing accounts for 80 percent of all antibiotic prescribing, even a small difference in efficacy can have huge implications,” Dr. Gerber said.
The second PCORI award received during fiscal 2013 supports the CHOP-led data network PEDSnet, which is comprised of children’s hospitals, data partners, and specialty networks. The PCORI contract, announced in December 2013, funds work to develop and expand PEDSnet as part of PCORnet: The National Patient-Centered Clinical Research Network.
PEDSnet combines a clinical data research network — including eight of the nation’s largest children’s hospital systems — with three condition-specific networks and two national data partners. CHOP’s Christopher Forrest, MD, PhD, serves as the principal investigator of PEDSnet.
PCORnet will be a secure, national data network that, according to PCORI, will improve the speed, efficiency, and use of patient-centered comparative effectiveness research. By integrating data available in the individual networks, PCORnet aims to provide access to a large amount of health information that can support a range of study designs.
Moreover, by enabling researchers and patients to interact directly and jointly determine research priorities, PCORnet aims to advance the shift in clinical research from investigator-driven to patient-centered studies.
“The Children’s Hospital of Philadelphia is thrilled to lend its efforts to PCORnet,” said Philip R. Johnson, MD, chief scientific officer and director of the Research Institute. “Multidisciplinary collaborations like this, that help researchers share findings and speed investigations, will help move innovative research from the bench to bedside and improve the care of children and families worldwide.”

Working in research reaps many rewards, including the understanding that the fruits of that work contribute to the collective scientific knowledge and inspire more research questions and discoveries. But perhaps the greatest reward for Children’s Hospital investigators comes in knowing that their research — whether in a clinic or laboratory — may improve the health of children across the globe.
The journey to that goal may be marked by honors and awards to CHOP investigators or for groundbreaking research programs. This year, Pennsylvania Bio, a biosciences global leader representing the “entire life sciences industry” in the Commonwealth, bestowed two prestigious awards on Children’s Hospital in recognition of its business and research innovations.
First, Children’s Hospital received the “Deal of the Year” award for its successful spinoff of gene company Spark Therapeutics. The award is intended for “a company that has promoted the growth of Pennsylvania’s bioscience industry by way of a substantial deal or strategic partnership,” according to PA Bio.
Based in part on the innovative work on adeno-associated virus vectors by Katherine A. High, MD, HHMI, and CHOP Research Institute’s Center for Cellular and Molecular Therapeutics, Spark Therapeutics was launched in October 2013 with a $50 million capital commitment from CHOP. A fully integrated gene therapy company, Spark is currently pursuing a Phase 3 program in blindness caused by mutations of the RPE65 gene, as well as a Phase 1/2 program in hemophilia B. The company is also involved in preclinical programs in neurodegenerative diseases and other hematologic disorders and forms of inherited blindness, according to its website.
The “Patient Impact Award,” given for contributions to the quality of healthcare or length of patients’ lives, was the second honor to Children’s Hospital from PA Bio this year. CHOP shared the award with the University of Pennsylvania for their joint immune therapy research program.
Led at CHOP by Stephan A. Grupp, MD, PhD, and at Penn by Carl H. June, MD, the immune therapy research team has been investigating using modified versions of patients’ own immune cells to attack — and destroy — tumors.
Last year the partnership led to dramatic, extraordinary results: Two children with acute lymphoblastic leukemia, the most common form of childhood leukemia, achieved a complete response after being treated with immune therapy. Since receiving the treatment, one of those patients remains healthy and cancer-free.
“The Children’s Hospital of Philadelphia is thrilled to be honored with these two awards,” said Philip R. Johnson, MD, chief scientific officer and director of the Research Institute and a new addition to the PA Bio Board of Directors. “They are a testament to the hard work of our investigators and staff, who work every day to improve the health of children.”